YOUR PRIVACY
To enhance your experience with our site, many of our web pages use “cookies” and shopper ID’s. Cookies are text files we place in your computer’s web browser to store your preferences. To find out more, read our updated privacy policy.
Teen Pregnancy FAQ
Teen pregnancy can be a difficult topic to broach — which is part of the reason it’s so rampant. In the communities we serve, more than 1 in 4 adolescent girls has had a pregnancy. To help explain why, here are some answers to our most frequently asked questions:
1. Why is teenage pregnancy so prevalent in the communities you serve?
In rural Maasai communities like the ones we serve, sexual activity often begins early — especially for girls. According to one survey, the average Maasai child begins engaging in sexual activity at age 10, compared to Kenya’s national average of 16. A key driver of this earlier sexual activity is child marriage. It is a common traditional practice amongst the Maasai, affecting 50% of girls in the communities we serve. When girls are married off at a young age, their sexual debut also occurs earlier. Traditions like these, combined with the inaccessibility of modern contraceptives, and lack of sexual and reproductive health education make adolescent girls in the communities we serve extremely vulnerable to early/teen pregnancies.
2. How did the COVID-19 pandemic exacerbate the issue?
In Kenya, almost 30% of students attend boarding schools. Like our schools, in addition to education they provide food, safety, and basic necessities. But when schools closed for an extended period during the pandemic, students returned home, where these needs, particularly for girls from impoverished households, went unmet. Lockdowns also caused further economic hardship on girls and their families, forcing many girls to resort to survival sex (see below) just to meet their basic needs.
Being away from the safety of boarding schools also meant returning to dangerous home environments for some, where contact with potential abusers increased. Across the country, reported sexual violence cases more than doubled among youth ages 10–17 during COVID-19 lockdowns. These various factors led to a 40% spike in teenage pregnancies across Kenya during the pandemic.
In response, we launched our Linda Dada campaign to spread awareness about reproductive health and safe sex practices, and reduce teen pregnancy through community-led dialogues, educational workshops, and local media campaigns.
3. What is survival sex?
Survival sex refers to transactional sex in exchange for money or basic necessities like food, shelter, and menstrual hygiene products. It is a common coping mechanism for women and girls living in extreme poverty and/or during times of crisis, such as the COVID-19 pandemic and Kenya’s recent drought. With our region’s inadequate contraceptive access and lack of sexual and reproductive health education, widespread survival sex creates higher rates of teen pregnancy. It also exposes girls to physical and sexual violence.
4. Why is contraceptive use so low in the communities you serve?
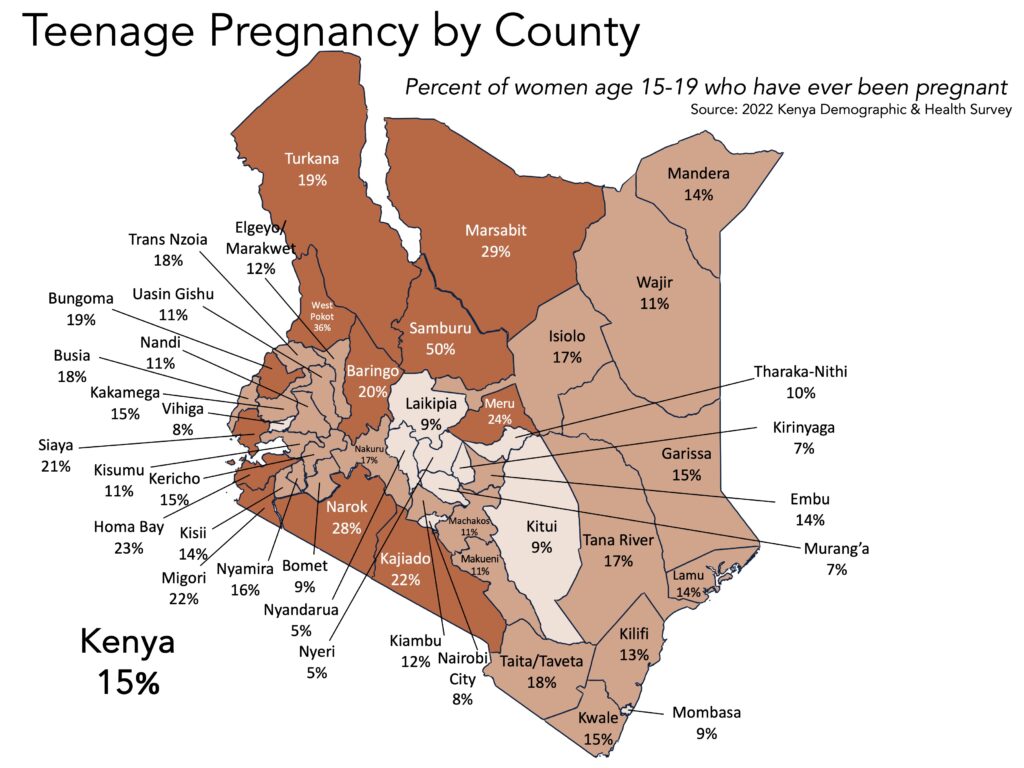
In Narok County (where the majority of our programming occurs), only 52% of married girls and women use modern contraceptives. This is due in large part to a lack of education and knowledge surrounding reproductive health (for example, less than 40% of Kenyan women have accurate knowledge of their ovulatory cycles).
Severe social stigma is another contributing factor to low contraceptive use. Studies have found that judgmental or negative attitudes of health workers are a major barrier to seeking sexual and reproductive healthcare, particularly among adolescents. This is one reason why opening our own youth-friendly health clinic was so critical. Core to our clinic’s mission is providing compassionate, discreet, and stigma-free care to adolescents.
Negative myths and misconceptions about family planning are fairly prevalent in the communities we serve, which also contribute to low contraceptive use. Some of these misconceptions about contraception include that it can cause serious adverse health effects, infertility, and birth defects, which is why educational health programs like ours are important. They dispel these myths and misconceptions about modern contraceptives, help people make informed decisions about their health, and increase safe sex practices and responsible contraceptive use.
Lastly, contraceptive use is low because contraception is also not easily accessible in our remote community. By one estimate, fulfilling unmet needs for modern contraceptives among Kenyan adolescents would decrease unintended pregnancies by 73%.
5. What are the health consequences of teenage pregnancy?
Globally, complications arising from pregnancy and childbirth are the leading cause of death for girls aged 15-19. Girls this age are twice as likely to die during childbirth as women 20 and older, as younger girls face higher risks of conditions like eclampsia, puerperal endometritis, and systemic infections during pregnancy. Adolescent mothers also face serious mental health consequences, as hormonal changes, stress, and social stigma during pregnancy are linked to mental health problems like depression and anxiety.
Girls aren’t the only ones at risk: babies born to adolescent mothers face higher rates of infant mortality and are more likely to develop chronic medical conditions and behavioral problems.
6. What is the typical outcome in life for teens who do become pregnant in the communities you serve?
In many Kenyan schools, students are suspended immediately once they become pregnant. Per national guidelines, they must also wait a minimum of six months after giving birth to return to school. During this extended time at home, girls not only fall behind in their studies, but also face stigma surrounding unwed pregnancy and greater pressure to marry. The pervasive expectation that girls and women stay home and raise children, combined with the financial burden of childcare, prevents many new mothers from ever completing their education. In turn, this limits their opportunities for economic advancement, often trapping them in a lifetime of poverty.
7. How does Kakenya’s Dream handle teen pregnancy with girls in your programs?
At Kakenya’s Dream, pregnant students are allowed to remain in school and live on campus until the last month of their pregnancy. They receive customized support from our full-time counselor during that time, as well as prenatal care. We also work with their parents/guardians to support their transition home before delivery. After the baby is born, we conduct regular home visits to ensure mothers and babies are doing well. Once childcare can be arranged, the mothers can return to school, where they receive extra one-on-one instruction to catch up on their missed studies.
